Diabetes and Oral Health: Tips for a Healthy Smile with How to Cure Diabetes

- Diabetes and Oral Health: Tips for a Healthy Smile with How to Cure Diabetes
- Diabetes and Oral Health Problems
- Type 2 Diabetes and Dental Health
- Dental Extractions and Diabetes
- Prevention and Care for Healthy Teeth and Gums with Diabetes
- The Role of Diabetes Care in Oral Health
- Diabetes and Gum Disease: Understanding the Link
- Oral Health Tips for Individuals with Diabetes
- Potential Oral Complications and Managing Risks with Diabetes
- Living with Diabetes: Your Oral Health Guide
- How to Cure Diabetes: Taking Charge of Your Oral and Overall Health
Diabetes and Oral Health: Tips for a Healthy Smile with How to Cure Diabetes
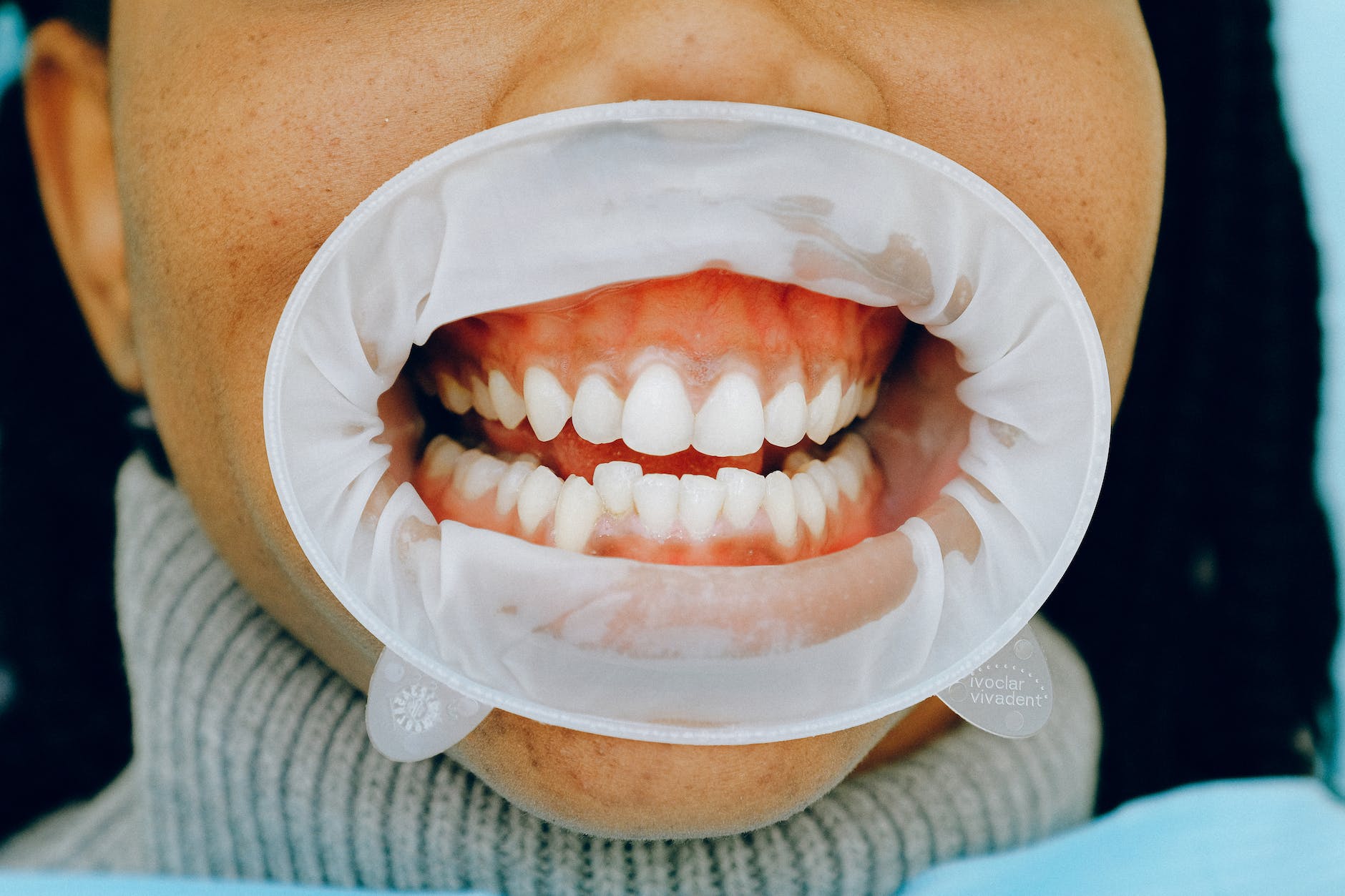
Diabetes and Oral Health are closely related. Proper management of blood sugar is crucial to prevent oral health problems for individuals with diabetes. High blood sugar levels weaken the immune system and increase the risk of gum diseases and cavities. Taking care of oral hygiene, including regular dental check-ups and practicing good oral habits, can help prevent complications. Learn more about the impact of diabetes on oral health and ways to maintain a healthy smile with How to Cure Diabetes.
Click to transform your health journey today!
Diabetes and Oral Health Problems
Diabetes and oral health are closely intertwined, and individuals with diabetes face a higher risk of experiencing oral health issues due to elevated blood sugar levels. Let's explore the impact of diabetes on oral health and the connection between blood sugar and dental issues.
Impact of Diabetes on Oral Health
Diabetes can have detrimental effects on oral health. Uncontrolled diabetes weakens the immune system, compromising its ability to fight infections in the mouth. This weakened immunity increases the likelihood of developing bacterial infections in the oral cavity.
Connection between Blood Sugar and Dental Issues
Elevated levels of sugar in saliva provide food for bacteria present in dental plaque. This increased sugar supply promotes the formation of cavities, tooth decay, and gum diseases. Maintaining optimal blood sugar control is crucial to minimize the risk of dental complications.
Increased Risk of Gum Diseases and Cavities
Individuals with diabetes are more susceptible to gum diseases such as gingivitis and periodontitis. Poorly controlled blood sugar levels can lead to persistent inflammation and delay the healing process of gum tissues. Additionally, the high sugar environment in the mouth can contribute to an increased risk of cavities.
To mitigate these risks, individuals with diabetes should prioritize preventive measures and adequate oral care. Regular dental visits, daily oral hygiene practices, and a healthy lifestyle play key roles in maintaining good oral health.
Visit our services page now!
Type 2 Diabetes and Dental Health
Type 2 Diabetes often leads to oral complications, emphasizing the importance of maintaining good oral health. Understanding the link between Type 2 Diabetes and oral health is crucial for effective management. Additionally, the effects of Metformin, a commonly prescribed medication for Type 2 Diabetes, on oral health need to be considered. By managing oral health effectively, individuals with Type 2 Diabetes can minimize the risk of oral complications and maintain a healthy smile.
Link Between Type 2 Diabetes and Oral Complications
Type 2 Diabetes has been associated with an increased risk of oral complications, especially gum diseases and infections. The elevated blood sugar levels in diabetes provide a favorable environment for bacteria to thrive, leading to a higher likelihood of gum diseases such as periodontitis. Diabetic individuals may also experience slower healing and increased susceptibility to oral infections. Maintaining optimal blood sugar control is essential to reduce the risk of these oral complications.
Effect of Metformin on Teeth
Metformin, a commonly prescribed medication for Type 2 Diabetes, has been found to have some impact on oral health. While Metformin itself does not directly cause tooth decay, it may contribute to the development of dry mouth as a side effect. Dry mouth increases the risk of cavities and other oral health problems. If you are taking Metformin, it is important to stay hydrated, practice good oral hygiene, and visit your dentist regularly to monitor and address any potential oral health issues.
Managing Oral Health with Type 2 Diabetes
Managing oral health plays a crucial role in maintaining overall well-being for individuals with Type 2 Diabetes. Here are some essential tips for managing oral health effectively:
- Monitor and control blood sugar levels through proper diabetes management.
- Practice good oral hygiene by brushing your teeth at least twice a day with a fluoride toothpaste and flossing daily.
- Use an antimicrobial mouthwash as recommended by your dentist to minimize oral bacteria.
- Visit your dentist regularly for professional cleanings, dental check-ups, and early detection of any oral issues.
- Maintain a balanced diet low in sugars and carbohydrates to reduce the risk of tooth decay.
- Avoid smoking, as it increases the risk of gum diseases and oral health problems.
- Inform your dentist about your diabetes status and any changes in medication or blood sugar control.
By following these strategies and being proactive in oral health management, individuals with Type 2 Diabetes can significantly reduce the risk of oral complications and maintain optimal oral health. Continue reading: Oral Health Tips for Individuals with Diabetes
Dental Extractions and Diabetes
Diabetic individuals may sometimes require dental extractions, also known as tooth removal. It is crucial to consider certain factors when it comes to dental extractions for patients with diabetes.
Considerations for Dental Extractions with Diabetes
When planning a dental extraction for a patient with diabetes, the dental professional needs to assess the patient's overall health and glycemic control. Factors to consider include:
- Current blood sugar levels
- Overall diabetes management
- Wound healing ability
- Potential complications due to anesthesia
Collaboration between the patient's dentist and primary care physician can provide valuable insights into the patient's overall health status and help determine the optimal timing for the dental extraction procedure.
Precautions and Post-Extraction Care for Diabetic Patients
After a dental extraction, diabetic patients may need to take additional precautions to ensure proper healing and minimize the risk of complications. It is recommended to:
- Maintain stable blood sugar levels before and after the procedure
- Follow any prescribed pre-medication regimen
- Be cautious with pain management medications, as some may contain sugars
- Adhere to a soft diet and avoid chewing on the extraction site
- Continue proper oral hygiene practices, excluding the extraction site
- Contact the dentist immediately if any unusual symptoms or complications arise
Good communication between the patient, dentist, and healthcare team ensures comprehensive care and reduces the risk of post-extraction complications. Managing blood sugar levels, adhering to any prescribed medications, and closely following post-extraction instructions are crucial in promoting optimal healing for diabetic patients.
Remember, it is essential for individuals with diabetes to consult with their healthcare team, including their dentist, to receive personalized guidance and recommendations based on their specific needs and diabetes management plan.
Prevention and Care for Healthy Teeth and Gums with Diabetes
When it comes to diabetes, maintaining proper oral hygiene is crucial for overall health. Diabetic individuals should pay special attention to their teeth and gums to prevent potential complications. This section will discuss the importance of daily oral hygiene routines, regular dental check-ups, and tips for managing dry mouth.
Importance of Daily Oral Hygiene Routine
Establishing a daily oral hygiene routine is essential for individuals with diabetes. Here are some key practices to incorporate:
- Brush your teeth at least twice a day using a fluoride toothpaste to prevent cavities.
- Use a soft-bristle toothbrush and gentle, circular motions to clean your teeth and gums.
- Don't forget to brush your tongue to remove bacteria and freshen your breath.
- Floss daily to remove plaque and debris from between your teeth.
- Rinse your mouth with an alcohol-free mouthwash to further reduce bacteria.
Regular Dental Check-ups for Diabetic Individuals
Regular dental check-ups are crucial for maintaining oral health, especially for individuals with diabetes. Here are some key considerations:
- Schedule dental visits every six months or as recommended by your dentist.
- Inform your dentist about your diabetes condition and any recent episodes of hypoglycemia.
- Discuss any concerns or changes in your oral health during these appointments.
- Allow your dentist to perform professional cleanings and take X-rays to monitor your oral health.
Tips for Managing Dry Mouth
Dry mouth, also known as xerostomia, is a common issue among individuals with diabetes. Here are some tips to help manage dry mouth:
- Stay hydrated by drinking plenty of water throughout the day.
- Chew sugar-free gum or suck on sugar-free lozenges to stimulate saliva production.
- Avoid tobacco and alcohol, as they can worsen dry mouth symptoms.
- Use over-the-counter saliva substitutes or mouth sprays as recommended by your dentist.
- Maintain proper oral hygiene to prevent infections and maintain oral health.
By following these preventive measures and maintaining good oral hygiene habits, individuals with diabetes can take proactive steps to ensure healthy teeth and gums. Remember to consult with your dentist for personalized advice tailored to your specific needs and diabetes management.
The Role of Diabetes Care in Oral Health
Blood Sugar Control and its Impact on Oral Health
Effective management of blood sugar levels plays a crucial role in maintaining optimal oral health for individuals with diabetes. Consistently high blood sugar levels can weaken the immune system, making individuals more susceptible to oral infections and gum diseases. Research shows a direct correlation between poorly controlled diabetes and increased risk of tooth decay, gum inflammation, and delayed wound healing in the mouth.
To mitigate these risks, it is essential for individuals with diabetes to prioritize regular monitoring of blood sugar levels and work closely with their healthcare team to establish a comprehensive diabetes care plan. By achieving and maintaining stable blood sugar levels, individuals can significantly reduce the potential negative impact on their oral health.
Collaborating with Your Dentist for Comprehensive Care
In addition to managing blood sugar levels, collaboration between individuals with diabetes and their dentist is vital for comprehensive oral health care. Dentists who specialize in treating patients with diabetes understand the unique challenges and potential complications associated with the disease.
During dental visits, it is crucial for individuals with diabetes to provide detailed information about their medical history, including their diabetes diagnosis, current medications, and any specific concerns related to their oral health. This open communication ensures that dentists can tailor their treatment plans and provide appropriate recommendations for ongoing care.
Working together, individuals with diabetes and their dentists can develop a personalized oral hygiene routine, which may include regular dental cleanings, specialized gum disease management, and targeted preventive strategies. Dentists can also provide guidance on the best dental products, such as toothpaste and mouthwash, to support optimal oral health.
By establishing a strong relationship with a trusted dentist, individuals with diabetes can receive comprehensive oral health care that addresses their unique needs and helps maintain a healthy smile.
Diabetes and Gum Disease: Understanding the Link
Gum disease, also known as periodontal disease, is a common condition that affects the gums and the surrounding tissues. This section explores the relationship between diabetes and gum disease, highlighting the connection and its implications for individuals with diabetes.
Exploring the Relationship between Diabetes and Gum Disease
Research has shown a strong association between diabetes and an increased susceptibility to gum disease. Individuals with diabetes are more prone to developing gum disease due to factors such as impaired blood sugar control and weakened immune function.
Diabetes affects the body's ability to utilize insulin effectively, leading to high blood sugar levels. Elevated blood sugar levels provide an ideal environment for bacteria to thrive in the mouth, leading to the formation of plaque and tartar. Over time, this accumulation of bacteria can cause inflammation and infection of the gums, resulting in gum disease.
Gum disease, in turn, can further complicate diabetes management. The chronic inflammation caused by gum disease can make it more challenging to control blood sugar levels, potentially leading to complications in diabetes management.
Managing Gum Disease Symptoms for Better Diabetes Control
Proper management of gum disease is crucial for individuals with diabetes to maintain better control of their diabetes and promote overall oral health. Here are some strategies for managing gum disease symptoms:
- Regular dental check-ups: Visit your dentist regularly for professional cleanings and thorough examinations of your gums. Your dentist can monitor the progression of gum disease and recommend appropriate treatments.
- Maintaining good oral hygiene: Practice proper oral hygiene habits, including brushing your teeth at least twice a day, flossing daily, and using an antiseptic mouthwash. This helps remove plaque and bacteria, reducing the risk of gum disease.
- Controlling blood sugar levels: It is essential for individuals with diabetes to manage their blood sugar levels effectively. Consistent blood sugar control can help reduce the severity and progression of gum disease.
- Quit smoking: Smoking not only increases the risk of gum disease but also complicates diabetes management. Quitting smoking can improve both oral health and overall well-being.
- Seek professional treatment: If gum disease has progressed, your dentist may recommend advanced treatments such as deep cleaning (scaling and root planing), antibiotic therapy, or gum surgery to restore gum health.
By actively managing gum disease symptoms, individuals with diabetes can improve both their oral health and diabetes control, leading to better overall well-being.Remember, proper oral care and regular dental visits are crucial for individuals with diabetes to prevent and manage gum disease effectively. By understanding the relationship between diabetes and gum disease and taking proactive steps, individuals with diabetes can take control of their oral health and overall well-being.
Oral Health Tips for Individuals with Diabetes
Maintaining a Balanced Diet to Support Oral Health
A well-balanced diet plays a significant role in promoting oral health for individuals with diabetes. Opt for nutrient-rich foods that are low in added sugars and carbohydrates to help keep blood sugar levels stable. Incorporate plenty of fresh fruits, vegetables, lean proteins, and whole grains into your meals. These foods provide essential vitamins and minerals that support gum health and overall oral well-being.
Daily Habits to Promote a Healthy Mouth with Diabetes
In addition to maintaining a balanced diet, there are specific daily habits you can adopt to promote a healthy mouth and manage your diabetes effectively:
- Brush and floss regularly: Brush your teeth at least twice a day with fluoride toothpaste and use dental floss once a day to remove plaque and food particles.
- Monitor blood sugar levels: Keep a close eye on your blood sugar levels and work with your healthcare provider to keep them within a healthy range. Stable blood sugar levels contribute to better oral health.
- Stay hydrated: Drink plenty of water throughout the day to combat dry mouth, a common side effect of diabetes. Dry mouth can increase the risk of tooth decay and gum disease.
- Avoid tobacco and limit alcohol consumption: Smoking and excessive alcohol consumption can worsen oral health conditions. Quitting smoking and drinking in moderation can significantly benefit your oral and overall health.
- Regular dental check-ups: Schedule regular dental visits for professional cleanings, examinations, and screenings. Inform your dentist about your diabetes and any changes in your health.
By incorporating these oral health tips into your daily routine, you can maintain good oral hygiene and minimize the risk of oral complications associated with diabetes. Remember, proper oral care is an essential component of managing your overall health with diabetes.
Potential Oral Complications and Managing Risks with Diabetes
Recognizing and Addressing Oral Infections
Individuals with diabetes are more susceptible to oral infections due to weakened immunity. It is crucial to recognize the signs of oral infections and address them promptly. Common symptoms include persistent bad breath, swollen or bleeding gums, mouth sores, and loose teeth. If you experience any of these symptoms, consult your dentist immediately for appropriate diagnosis and treatment.
Strategies for Preventing Tooth Decay and Gum Problems
Preventing tooth decay and gum problems is vital for individuals with diabetes. Here are some strategies to consider:
- Maintain a thorough oral hygiene regimen: Brush your teeth at least twice a day with fluoride toothpaste and use dental floss daily to remove plaque buildup.
- Monitor your blood sugar levels: Keeping your blood sugar levels well-controlled can help reduce the risk of dental complications.
- Limit sugary foods and beverages: High sugar intake can contribute to tooth decay. Opt for healthier snack options and drink water or unsweetened beverages instead of sugary drinks.
- Quit smoking: Smoking not only increases the risk of gum disease but also hampers diabetes control. Seek support from healthcare professionals to quit smoking.
- Stay hydrated: Drink plenty of water to combat dry mouth, which can increase the risk of tooth decay and oral infections.
- Regular dental check-ups: Schedule regular dental visits for professional cleanings, exams, and early detection of any oral health issues.
By following these strategies, individuals with diabetes can actively manage the risks of tooth decay and gum problems, promoting optimal oral health alongside their diabetes management.
Living with Diabetes: Your Oral Health Guide
Living with diabetes requires being proactive in managing your oral health. Educating yourself about the potential effects of diabetes on your mouth and incorporating proper dental care into your diabetes management routine can help you maintain a healthy oral environment. This section provides valuable information and tips to guide you in balancing your diabetes and oral health needs.
Educating Yourself about Oral Effects of Diabetes
Understanding the impact of diabetes on your oral health is essential for comprehensive care. Here are some key points to be aware of:
- Dry Mouth: Diabetes can cause a decrease in saliva production, leading to dry mouth. This condition can increase the risk of tooth decay and oral infections.
- Gum Disease: Individuals with diabetes are more susceptible to gum disease due to compromised immune function. It is important to be aware of the signs and symptoms of gum disease, such as redness, bleeding, and swollen gums.
- Delayed Healing: Diabetes can hinder the healing process, including oral tissue healing. This can affect the recovery of oral surgeries or gum treatments.
- Thrush: Candida albicans, a type of fungus, can overgrow in the mouth, leading to oral thrush. Diabetes can create an environment conducive to fungal infections like thrush.
Tips for Incorporating Dental Care into Diabetes Management
To maintain optimal oral health while managing your diabetes, here are some helpful tips:
- Maintain Good Blood Sugar Control: Keeping your blood sugar levels within the target range can reduce the risk of oral complications associated with diabetes.
- Brush and Floss Regularly: Practice proper oral hygiene by brushing your teeth at least twice a day with fluoride toothpaste and flossing daily. This helps remove plaque and bacteria, reducing the risk of gum disease and tooth decay.
- Visit Your Dentist Regularly: Schedule regular dental check-ups, ideally every six months, to monitor your oral health, address any issues early on, and receive professional cleanings.
- Communicate with Your Healthcare Team: Inform both your dentist and primary care physician about your diabetes status and any changes in your blood sugar control. This collaboration ensures comprehensive care tailored to your needs.
- Manage Dry Mouth: Stay hydrated, avoid excessive caffeine and alcohol, and consider using artificial saliva or sugar-free gum to stimulate saliva production. Consult with your dentist for additional recommendations.
- Quit Smoking: Smoking increases the risk of gum disease and oral infections. If you smoke, talk to your healthcare team about strategies and resources to quit smoking.
By educating yourself about the oral effects of diabetes and implementing proper dental care strategies, you can navigate the relationship between diabetes and oral health more effectively, promoting a healthier smile and overall well-being.
How to Cure Diabetes: Taking Charge of Your Oral and Overall Health
When it comes to managing diabetes, taking care of your oral health is just as important as controlling your blood sugar levels. By adopting healthy habits and following specific guidelines, you can significantly reduce the risk of oral complications associated with diabetes.
Tips for Maintaining Excellent Oral Health
- Brush your teeth at least twice a day using fluoride toothpaste to remove plaque and prevent tooth decay.
- Floss daily to clean between your teeth and along the gumline, where a toothbrush cannot reach.
- Use an antimicrobial mouthwash to reduce bacteria in your mouth and prevent gum diseases.
- Avoid smoking or using tobacco products, as they can worsen oral health problems.
- Limit your consumption of sugary and acidic foods and beverages, as they can contribute to tooth decay.
- Stay hydrated to combat dry mouth, a common side effect of diabetes medication.
Regular Dental Visits for Optimal Oral Health
Make sure to schedule regular dental check-ups with your dentist, ideally every six months. These visits are essential for monitoring your oral health, detecting any potential issues early on, and receiving professional cleanings to remove plaque and tartar buildup. During these appointments, inform your dentist about your diabetes and any changes in your medical condition.
Collaborating with Your Healthcare Professionals
It's crucial to communicate with both your dentist and your primary care physician about your diabetes management. They can work together to develop a comprehensive care plan that accounts for your overall health and its impact on your oral well-being. Be sure to inform them about any medications you are taking and follow their recommendations for optimal health.
By following these guidelines and making your oral health a priority, you can take charge of your diabetes and ensure a healthier smile. Remember, proper oral care is a vital component of your overall well-being and can significantly contribute to your overall quality of life.
- Comprehensive Guidelines for Effective Diabetes Management - Your Key to Conquering Diabetes
- Gut Microbiome Modulation: The Key to Managing Diabetes in the US
- Relieve Persistent Thirst with How to Cure Diabetes: Effective Solutions for Unquenchable Thirst in the US
- Addressing childhood obesity today to protect the health of future generations
- Live Well Minute: Mastering Diabetes Management


